What is malaria?
Malaria is one of the most devastating mosquito-borne illnesses in the world. While mild cases cause little more than severe flu-like symptoms, severe cases lead to a painful death. According to the CDC, there were approximately 219,000,000 cases of malaria worldwide in 2010. Of these, 660,000 died as a result of the disease; 91% of these people lived in sub-Saharan Africa. Nearly all of the approximately 15, 000 cases of malaria diagnosed each year in the US were contracted when the patients were visiting or living in parts of the world where malaria is endemic, especially Africa and southern Asia.
How do people get malaria?
Like the other diseases described here, malaria is caused by the bite of an infected mosquito. There are important differences between malaria and the other diseases.
- Malaria is caused by a parasitic protist, more specifically, a single-celled eukaryotic organism (in layman's terms, a single-celled organism that is more complex than a bacterium). Medically, this is important because this type of organism requires different treatment strategies than does a virus.
- Humans are the definitive host of the malaria parasite. The viruses that cause West Nile encephalitis, etc., are best adapted to reproduce in non-human hosts. This may be why there is usually a high percentage of infections that create no symptoms. In contrast, the malaria parasites are adapted specifically to live in humans. The term "definitive host" means that the parasite undergoes most of its development and usually reaches sexual maturity in that host. What all this means is (a) the malaria parasite is very efficient at infecting humans, and (b) mosquitoes can spread the disease from person to person without the need for an intermediate host such as a bird or small mammal.
What is the malaria parasite?
The parasitic protists that cause malaria are four species of the genus Plasmodium.
- Plasmodium falciparum
- P. vivax
- P. ovale
- P. malariae
- P. falciparum causes the most deadly form of malaria
- P. vivax and P. ovale cause infections that can go through years-long periods of remission and shorter periods of relapse.
Which mosquitoes carry the malaria parasite?
Only certain species of the genus Anopheles are vectors that can transmit Plasmodium to humans. In Virginia, only one of the three common species of Anopheles, A. quadrimaculatus, is a vector of malaria.
Copyright Tom Murray, 2007. Used under a Creative Commons Attribution-NoDerivs-NonCommercial 1.0 Generic License.
What happens during infection?
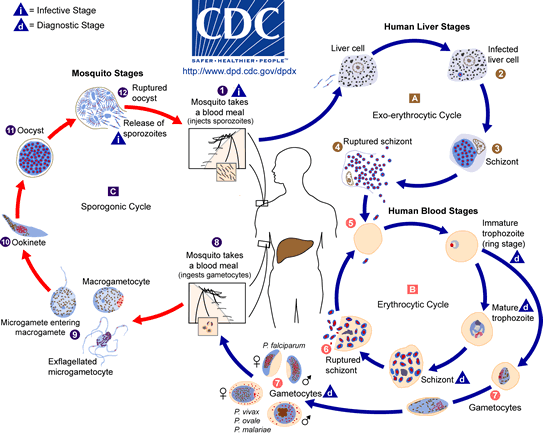
The life cycle of Plasmodium is very complex, involving a number of distinct developmental stages. Presented here is a "big picture" view of Plasmodium infection in humans and mosquitoes, especially as it relates to the symptoms of malaria.
Those of you who are interested in more details of the intricate life cycle of these parasites can find more information on the Plasmodium life cycle page. Even more detail can be found on the Blood-borne Protozoa page from the University of South Carolina School of Medicine. The This Week in Parasitology podcast about the Plasmodium life cycle may also be of interest.
The bite. Infection starts with the bite on an infected mosquito. When a mosquito bites, its goal is to drink blood that is necessary for her to lay eggs. A mosquito ejects saliva into the host's blood to prevent the it from clotting while feeding. Plasmodium living in the salivary gland of the mosquito are passed to the host in the saliva.
Infection of the liver. These single-celled parasites travel through the bloodstream until they reach the liver. The parasites enter liver cells and move to the next stage of their life cycle. The cells multiply and develop into two new forms. Some of the cells develop into a form that infects red blood cells. Others develop into a form that can infect mosquitoes.
Infection of the blood. Plasmodium cells burst out of the liver and infect red blood cells. It is at this point that the typical symptoms of malaria develop: fever, chills, aches, anemia, etc. The parasite multiplies in the red blood cells until the host cells burst, allowing the amplified parasite to infect even more red blood cells. The red blood cells all break open at about the same time (as opposed to a constant low-level bursting of cells). This accounts for the periodic nature of malarial symptoms: Symptoms appear suddenly and intensely as one round of red blood cells are destroyed, then recede until the next round of blood cell destruction. The exact timing of the cycle of appearance and relief of symptoms depends on the species of Plasmodium involved.
Infection of mosquitoes. If a mosquito of the right species bites a person with malaria, they can ingest and become infected with Plasmodium. Once in the mosquito, Plasmodium undergoes another series of changes that include sexual reproduction, infection of the gut, and infection of the salivary glands. Once in the salivary glands, the parasites can be transmitted to another human host.
Those of you who are interested in more details of the intricate life cycle of these parasites can find more information on the Plasmodium life cycle page. Even more detail can be found on the Blood-borne Protozoa page from the University of South Carolina School of Medicine. The This Week in Parasitology podcast about the Plasmodium life cycle may also be of interest.
The bite. Infection starts with the bite on an infected mosquito. When a mosquito bites, its goal is to drink blood that is necessary for her to lay eggs. A mosquito ejects saliva into the host's blood to prevent the it from clotting while feeding. Plasmodium living in the salivary gland of the mosquito are passed to the host in the saliva.
Infection of the liver. These single-celled parasites travel through the bloodstream until they reach the liver. The parasites enter liver cells and move to the next stage of their life cycle. The cells multiply and develop into two new forms. Some of the cells develop into a form that infects red blood cells. Others develop into a form that can infect mosquitoes.
Infection of the blood. Plasmodium cells burst out of the liver and infect red blood cells. It is at this point that the typical symptoms of malaria develop: fever, chills, aches, anemia, etc. The parasite multiplies in the red blood cells until the host cells burst, allowing the amplified parasite to infect even more red blood cells. The red blood cells all break open at about the same time (as opposed to a constant low-level bursting of cells). This accounts for the periodic nature of malarial symptoms: Symptoms appear suddenly and intensely as one round of red blood cells are destroyed, then recede until the next round of blood cell destruction. The exact timing of the cycle of appearance and relief of symptoms depends on the species of Plasmodium involved.
Infection of mosquitoes. If a mosquito of the right species bites a person with malaria, they can ingest and become infected with Plasmodium. Once in the mosquito, Plasmodium undergoes another series of changes that include sexual reproduction, infection of the gut, and infection of the salivary glands. Once in the salivary glands, the parasites can be transmitted to another human host.
How is malaria diagnosed?
Different stages of Plasmodium may be identified by blood tests of potential malaria patients. In addition, more sensitive tests such as PCR (polymerase chain reaction, a way to detect the presence of Plasmodim DNA in a patient) or immunological tests (detection of Plasmodium through use of antibodies, or detection of anti-Plasmodium antibodies made by a patient) may be used.
Despite the existence of a variety of tests, malaria can be surprisingly difficult to diagnose, both in the US and in countries where malaria is endemic. In the US, where malaria is very rare, doctors may not think to order the appropriate tests. In places where malaria is common, there are many people who have developed partial immunity from previous infections. They have sufficient immunity to avoid malarial symptoms, but insufficient immunity to avoid infection entirely. As such, they may carry a chronic low-level infection, and the presence of Plasmodium in a patient may be irrelevant to their current illness. For these individuals, more sophisticated testing of the amount of parasite in the blood may be necessary for an accurate diagnosis.
Despite the existence of a variety of tests, malaria can be surprisingly difficult to diagnose, both in the US and in countries where malaria is endemic. In the US, where malaria is very rare, doctors may not think to order the appropriate tests. In places where malaria is common, there are many people who have developed partial immunity from previous infections. They have sufficient immunity to avoid malarial symptoms, but insufficient immunity to avoid infection entirely. As such, they may carry a chronic low-level infection, and the presence of Plasmodium in a patient may be irrelevant to their current illness. For these individuals, more sophisticated testing of the amount of parasite in the blood may be necessary for an accurate diagnosis.
How is malaria treated?
Once a diagnosis of malaria has been confirmed, the parasite may be tested for drug resistance. In other cases, drug resistance may be inferred based on where the patient became infected (Plasmodium strains from certain geographic areas tend to differ in terms of specific types of drug resistance).
Most drugs used to treat malaria are specific for the developmental stage that infects and destroys red blood cells. These drugs include quinine and a number of quinine derivatives.
Another quinine-related drug, primaquine, is specific for the stage of Plasmodium that infects liver cells. Also, antibiotics related to tetracycline, especially doxycyline, may be administered in conjunction with standard anti-malarial drugs.
The exact treatment depends on a number of factors, including
Most drugs used to treat malaria are specific for the developmental stage that infects and destroys red blood cells. These drugs include quinine and a number of quinine derivatives.
Another quinine-related drug, primaquine, is specific for the stage of Plasmodium that infects liver cells. Also, antibiotics related to tetracycline, especially doxycyline, may be administered in conjunction with standard anti-malarial drugs.
The exact treatment depends on a number of factors, including
- The Plasmodium species
- The severity of the symptoms
- The age of the patient
- Other health factors (concurrent illness, weight, pregnancy, etc.)
- Availability of treatment
Is there a malaria vaccine?
Despite decades of research, there is no vaccine for malaria. Among several possible vaccines in development is the RTS, S vaccine. Early results of Stage III clinical trials were published in the New England Journal of Medicine. It is possible that the vaccine will be licensed for use within the next few years.
Beyond concerns of safety and efficacy, there are also concerns regarding the cost of a malaria vaccine. A cost-effectiveness analysis published in Malaria Journal concludes that the RTS, S vaccine is very cost effective compared to the main current preventative strategy, the use of long-lasting insecticide-treated nets.
Beyond concerns of safety and efficacy, there are also concerns regarding the cost of a malaria vaccine. A cost-effectiveness analysis published in Malaria Journal concludes that the RTS, S vaccine is very cost effective compared to the main current preventative strategy, the use of long-lasting insecticide-treated nets.
Who is most at risk?
Anyone bitten by an infected mosquito is at risk for developing malaria, but the majority of deaths occur in children.